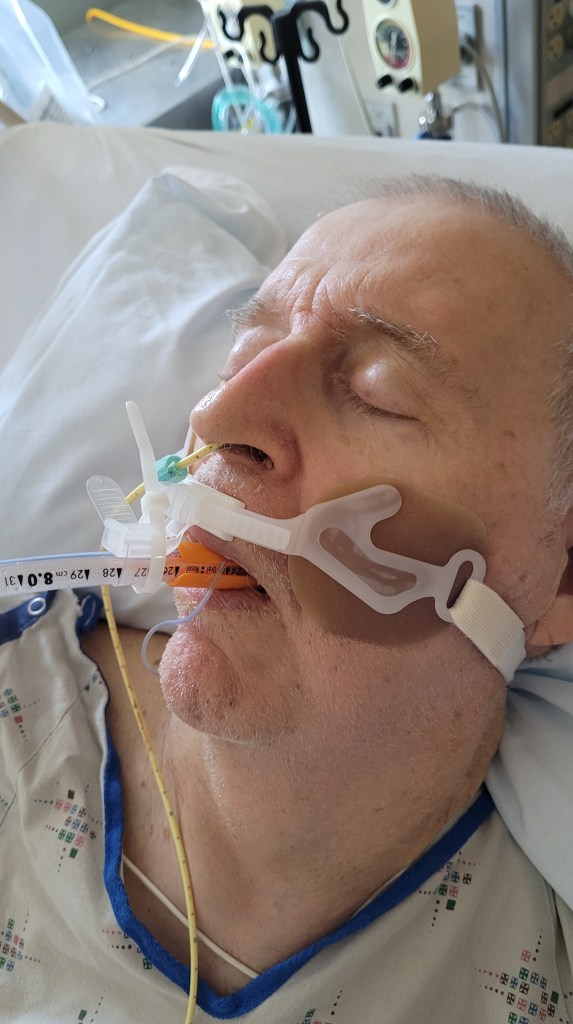
Dennis was in the ICU for 27 days. I felt like I was there too, and I was, nearly every day. Of course, the respiratory arrest and having to go on the ventilator was the worst complication of his stroke. The other important issue was his blood pressure, which was probably the cause of his stroke. That had to be stabilized to prevent another brain hemorrhage.
Unfortunately, unstable blood pressure has been one of Dennis’s problems for a long time, and was probably one of his first symptoms of Lewy Body Dementia. The IV med he was given right away, worked very well but as the amount was reduced, he would begin to have episodes of hypertension again and it would be increased. Eventually he was started on an oral med that was crushed and given through the nasogastric tube. When that didn’t take care of the spikes he was put on a second oral med. Then the amount of the first med was doubled. By his last day in ICU he was taking Norvasc 10 mg, Coreg 6.25 mg, Ismo 10 mg, Cozaar 100 mg, and a diuretic, Lasix 20 mg – all of which were for his blood pressure. Pretty impressive for a man who doesn’t like to take pharmaceuticals. He still has a spike now and then, but it was decided that he could have a higher “normal” as long as it didn’t result in 225/125, like it was on the night of his stroke.
Having weaned off the ventilator and having stabilized blood pressure readings for a couple of days, he was given a second swallowing evaluation. He didn’t do very well. That means he will be a long term tracheostomy patient to protect his lungs. It means it is still not safe for eating or drinking, two of his only remaining pleasures in life. But medically he was ready to move to a step down unit.
Every change causes some measure of anxiety. For me, the worry was that he wouldn’t be able to get help when he needed it on a unit with higher census and less staff. He still wasn’t able to move either arm enough to find a call light. He wasn’t able to move himself in bed at all. He couldn’t turn his head to see anything he tried to locate, he couldn’t speak unless someone deflated his trach cuff and placed the PMV valve. He was often lethargic, but becoming more aware of aches, pains, stomach rumblings and the need to cough.
I was called one night at home and told that he had been moved to a medical unit on another floor. The nurse working with him informed me that he was on the same kind of monitoring as in the ICU, and had a private room with a camera that allowed supervision at the nurse’s station. It actually sounded pretty good to me, and I was glad that he would be in a private room where it would be quiet and less confusing. I visited the next morning and was very pleased with his proximity to the nurse’s station and the attitude of the staff taking care of him. We practiced using a squeeze ball call system until he could work it correctly, and the PA directing his care gave permission for him to have the PMV valve in as long as he could tolerate.
There are always more mountains to climb however. The PA also told us that his inability to manage his secretions meant that he would need a more long term solution to nutrition and meds. The nasogastric tube could be replaced with a PEG feeding tube going directly into the stomach. This might also help his ability to swallow since it would mean one less tube going down his throat. He and I both felt this would be an improvement, although it will mean another exposure to anesthesia. It will take place tomorrow. I hope it won’t put him back into lethargy and brain fog, since we have just begun to make progress to more wakefulness and clarity.
In the back of my mind is the question of where he will be taken care of after hospitalization. They are already talking about nursing home placement and I know this is not going to be fun.