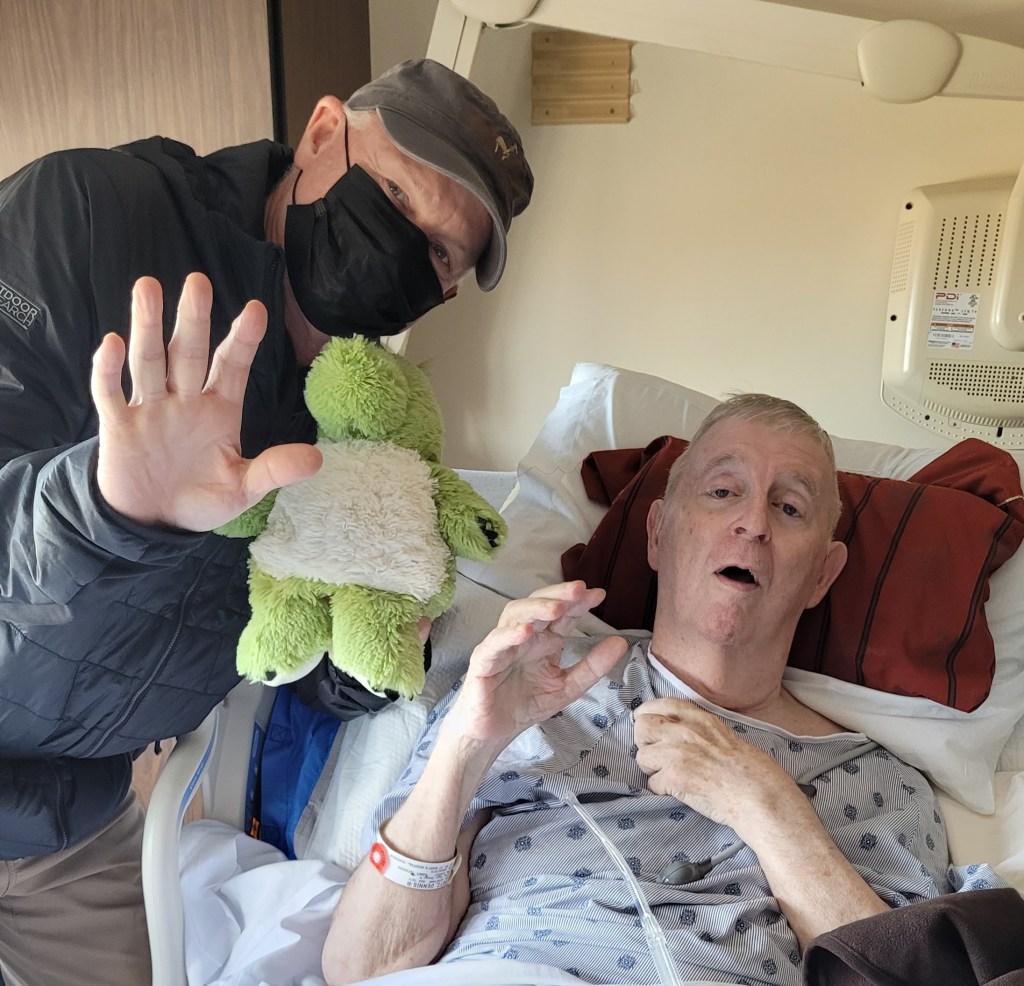
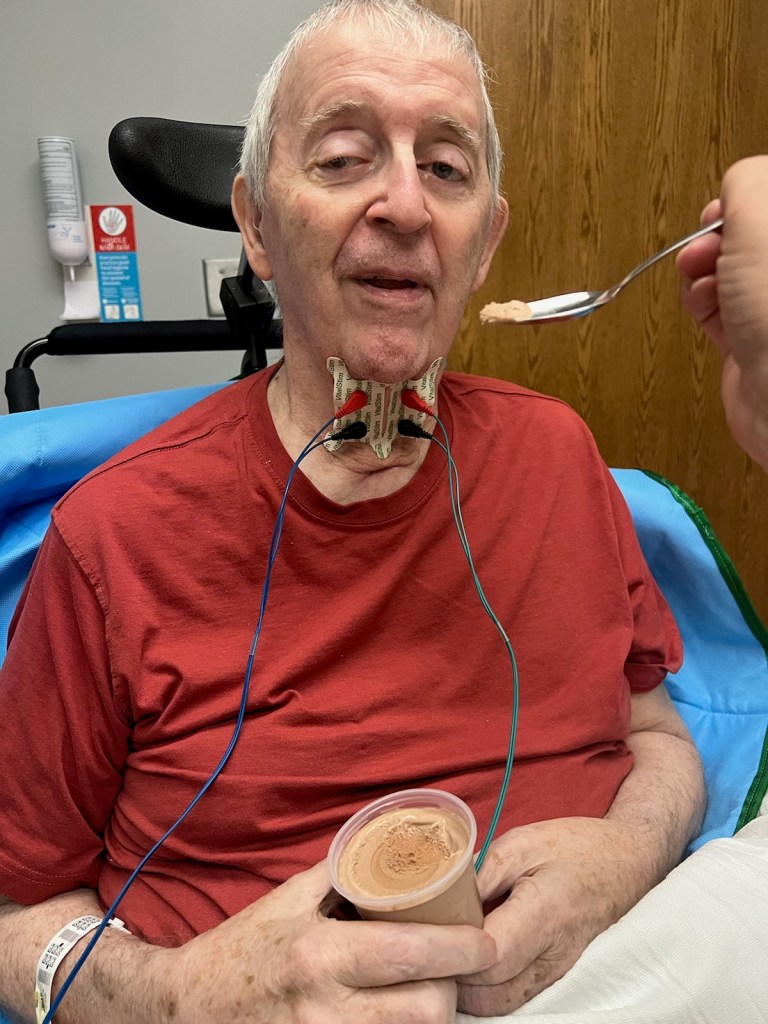
Because no damage was done, I will start with this event which I found somewhat humorous. Before I got to Maple Ridge yesterday, I received a call which started “I need to tell you what happened yesterday afternoon.” That’s not usually going to be a good report.
As it happened someone had left the control for the lift recliner where Dennis could find it. He often feels that making the chair go up and down relieves the burning sensation on his backside. This time it did more than that, as he lifted himself up and slid out of the chair. They had to pick him up off the floor with the lift. There were no bruises or pains as a result, and he looked fine to me when I arrived. I was grateful nothing had ruined our departure which took place a couple hours later.
They called all the staff, over the loudspeaker, to come say goodbye. Evidently that is a common ritual for this kind of facility.
A very resourceful friend found a tilt-in-space wheelchair for us – for free, no less. This made it possible to go home in a wheelchair van which was much less expensive than a stretcher by ambulance. The thirty minute trip was uneventful. I’m going to say that the driver left the minute we went through the front door at home because he didn’t even want to get asked to help. Not that I would have asked him.

The reality of being alone with my helpless husband had a hint of panic associated with it, I admit. But I hooked him up to the rented Hoyer lift and promptly found that it did not lift him high enough to easily leave the wheelchair. Another discovery was that he was not going in the recliner where I had envisioned him spending half of each day. It was too wide for the legs of the Hoyer.
It wasn’t a situation quite as bad as someone having to lift a car off a trapped passenger, but I was surprised that I was able to get him on the side of the bed, unhook the Hoyer, and finally get him straight and lying down. Surprised and tired. It was interesting how he was silent, bent nearly double in the sling, during the whole event. I think God has blessed him with limited awareness of any of the situations he’s in.
He and the cat “re-bonded” immediately, which was very nice to see. He also requested coffee with cream as soon as I had raised the head of the bed.
The rest of the evening was spent putting things away, trying to remember where I had put the things already put away, figuring out the medication and feeding schedule, and meeting a new caregiver who came at 6 pm for a couple of hours. More about that another time.
Since I had never spent a night with him since his “healthcare incarceration”, I did feel the need to sleep close by so I could see how he behaved. That is to say that I did not sleep much but spent most of the night listening to various levels of gurgling and snoring. I think I have learned that he remains quite still and does well when the head of the bed is raised. I believe he had a good night’s rest, but I decided not to ask him just in case. It was enough that he remained alive after his first night at home. We did it.