All in all, a good week.
Today, after a morning of various therapies, Dennis was helped into bed and got a much needed nap. As I watched him sleep, it was clear to me that he has improved. Even his appearance is more calm, less anxious, peaceful.

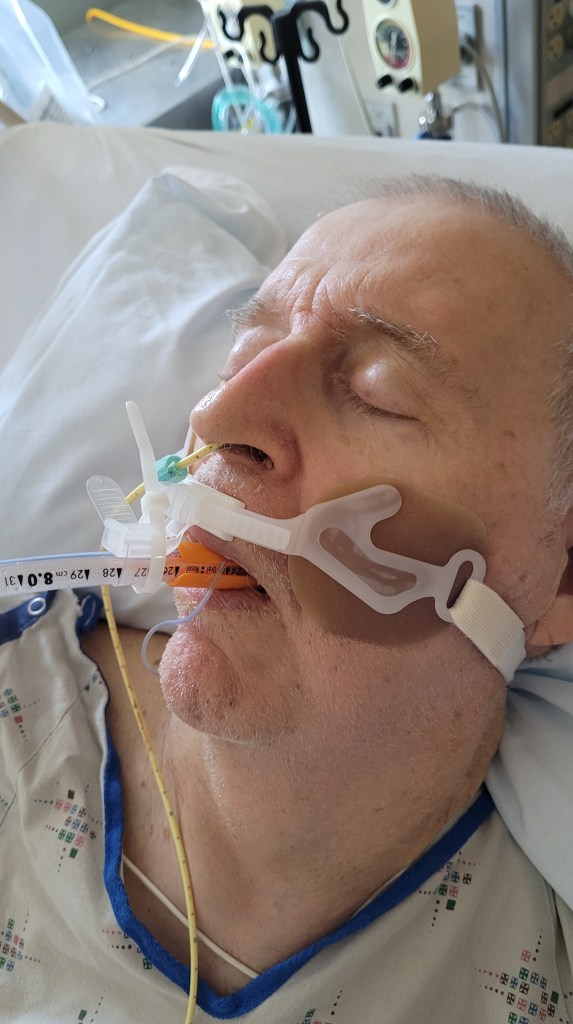
The biggest change came on Wednesday morning when respiratory therapy came into the room and swapped his trach out for a smaller, less irritating Jackson trach. When plugged, it does not allow air in or out, making the breathing experience about the same as not having a trach at all. It is still there if difficulties arise, but if all goes well for at least 48 hours, it is safe to remove it and let the tracheotomy heal up. There have been no difficulties. Saturday morning the trach is coming out and Dennis is so excited! It was the first thing he told me when I arrived this morning.
His voice has been more clear and easy to understand.
He has not needed suctioning to clear his airway.
He is moving his head and neck more, keeping a more normal position.
The progress on the physical therapy side is slower. He has continued to have low blood pressure when sitting and using the standing machine, making it hard for them to get him strong for those activities. Several times they have cut the session short and returned him to bed to rest. There is progress, but because Miller Dwan is an acute rehab facility, and Dennis’s problems are more chronic, there is once more talk about moving him to a sub acute facility to give more rest time to get stronger. This makes me nervous, but I am grateful for all they have done, their good communication with both the husband and me, and the excellent treatment he has had.
They wanted to have the trach out before they sent him elsewhere, and I have asked if they could also get him past needing the feeding tube. I am hopeful they will keep him another week. Social services will start looking for a facility closer to our home that could take him. I will start preparing our home in case there is no good place available.
In all this, I am not going to waste time and energy being fearful about problems we don’t even know we have yet. I want God to know that I trust him to work things out, when we have the need. I believe he always has a plan for our ultimate good. The only difference from day to day is that sometimes we see how the plan is good, and sometimes we don’t see – yet. His plan does not require me to be “in the know” at every step, and I clearly am not…
Sayings:
Nurse: “I need to take your blood pressure. Can I have this arm?” (the left one that he has trouble moving at all)
Dennis: “Yes, if you give it back when you’re done. I hardly use it anyway.”